Eye diseases
Retinal detachment
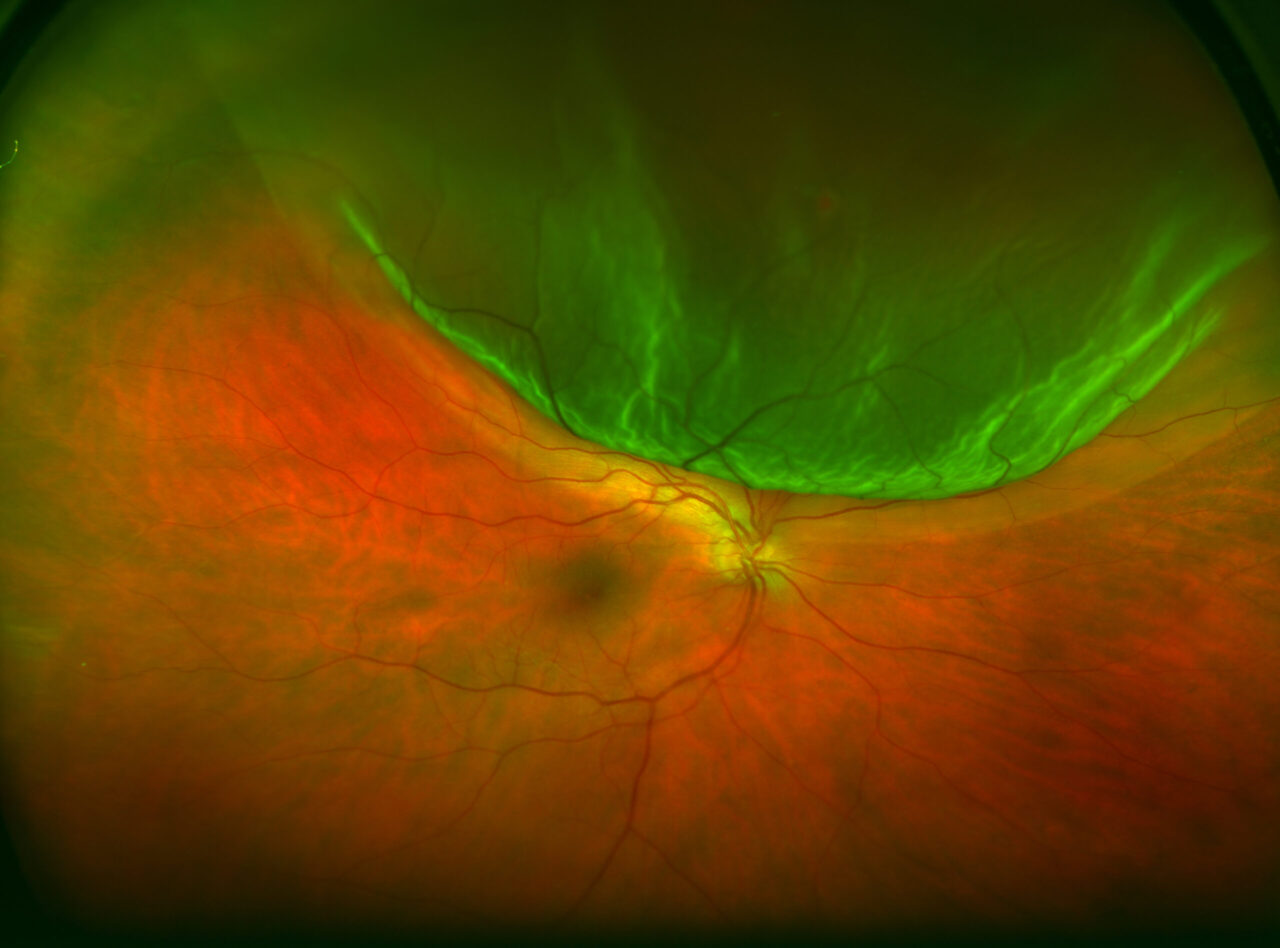
What is retinal detachment?
Retinal detachment consists of the separation of the retina (later that covers the inside of the eye) from the wall of the eye to which the choroid (the intermediate layer of the eyeball) is “stuck”.
Without the nutrients and oxygen received from the choroid, the highly specialist retinal cells that are unable to regenerate are damaged and cannot work properly. Therefore, vision loss could be very severe if it is not treated in time, and this is considered an ophthalmological emergency.
According to the mechanisms causing retinal detachment, there can be several types:
- Rhegmatogenous retinal detachment: this is the most frequent and is caused by the formation of small tears in the retina through which fluid can pass that “detaches” the retina.
- Tractional retinal detachment: this is caused by membranes, generally fibrous or fibrovascular, that pull on the retina and separate it from the choroid.
- Exudative retinal detachment: this occurs in inflammatory processes affecting the eye and can sometimes be due to the growth of new vessels in the vascular layer of the choroid, causing the retinal to lift slightly.
Symptoms
Causes and risk factors
Diagnosis
Treatment
This eye disease does not hurt, but you should pay attention to certain warning signs that are common to vitreous detachment and that might precede possible retinal detachment, such as the appearance or increase in floaters and flashes. Also, if you see a dark area or a black curtain over some part of your visual field, either at the top, bottom or on the sides, retinal detachment might have already occurred. In cases where the central and most important area of the retina is affected, you might also notice distorted images and loss of visual acuity.