Treatments
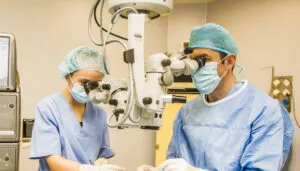
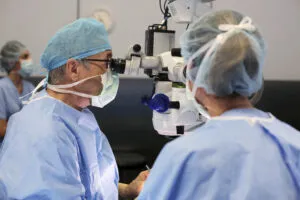
Vitreoretinal surgery
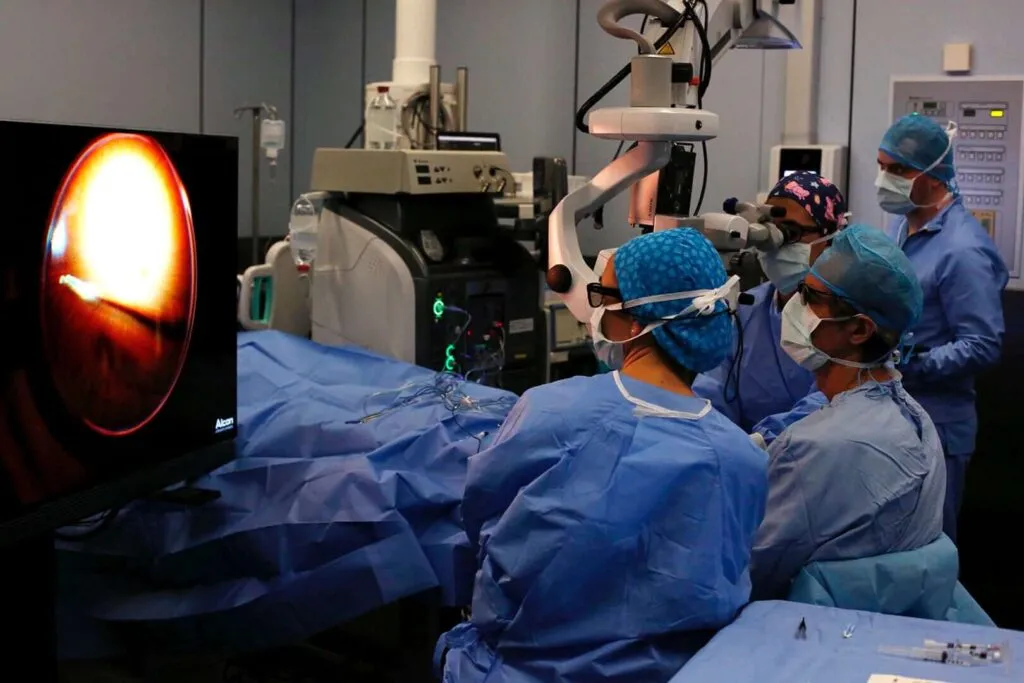
What does the retina operation consist of?
Vitreoretinal surgery includes various ocular microsurgery techniques intended to act on the vitreous gel (gelatinous liquid that fills the eyeball) and the retina (innermost later of the eye where light stimuli is transformed into nerve impulses transmitted to the brain for interpretation).
The retina is a very complex and highly specialised tissue and its good health and function is essential for us to be able to see. Therefore, advances in this surgical field have been essential for avoiding many cases of blindness.
In recent years, technological innovation has allowed the use of increasingly smaller instruments to access the inside of the eye through minimal incisions and the performance of less traumatic operations, achieving better visual results and minimising the risk of complications. In addition, high-speed vitrectomy has been introduced and innovative technologies are being developed which, using ultrasound, “liquefy” the vitreous gel instead of cutting it mechanically. To achieve the greatest precision in surgical procedures, the visualisation of the intraocular structures has also been improved thanks to equipment such as intraoperative OCT (a diagnostic test performed during surgery) or revolutionary 3D surgery systems.
Techniques
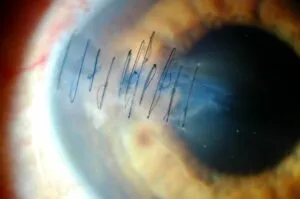
The vitrectomy, a technique in which the specialists at Miranza have been national experts for more than 30 years, is the main vitreoretinal surgery. However, there are other procedures we can use, such as scleral surgery for some cases of retinal detachment. A good surgical indication and the expert performance of the different types of retinal operation will allow the achievement of the best results in each case.
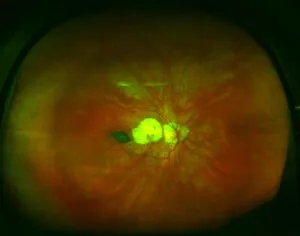
Diseases treated by retinal surgery
A large part of retinal diseases require surgery which, when performed early and expertly, can save many patients’ sight. In addition, vitreoretinal surgery is also indicated for the treatment of alterations to the vitreous gel (such as dense haemorrhages), problems derived from eyes with high myopia –with a 40% higher risk of suffering retinal damage- or complications associated with uveitis.
Recovery
Recovery varies based on your disorder and the retinal surgery technique used although, in many cases, these are procedures performed with local anaesthesia which do not require hospital admission.
Although you may notice some eye discomfort at first, this will soon subside with the help of the treatment we prescribe. You will also notice your vision gradually stabilising since you won’t achieve maximum visual quality immediately; this will take several weeks.
It is important that you follow the post-operative guidelines given, as well as any basic recommendations, and avoid sudden movements or physical effort during the first month. However, with the exception of a few precautions, you can resume your normal life and daily activities. Your evolution will be monitored during the appropriate follow-up visits.