Intravitreal injections prove effective in slowing progression of diabetic retinopathy
“The new treatment will improve patients’ vision by replacing laser photocoagulation, which is effective but causes scarring in the retina that reduces vision.”
Along with World Diabetes Day, which is held on 14 November, Dr Mónica Asencio, a retina specialist at Miranza IOA, announces a new effective treatment to halt the progression of diabetic retinopathy, the most common ocular complication of diabetes. According to the specialist, “luckily, we havean important new development in approaching diabetic retinopathy, which consists of the application of intravenous injections of antiangiogenic drugs as a new strategy to halt the progression of the disease.”
As Dr Asencio explains, “we have been using this treatment for a decade and a half for macular degeneration (AMD), as well as to treat diabetic macular oedema, the leading cause of vision loss in diabetic patients.” The new development, according to the ophthalmologist, is that recent studies have shown that injections applied to all patients suffering from the disease – and not only to 25% of them, who are those suffering from macular oedema – are capable of halting the progression of diabetic retinopathy with the same effectiveness as the reference treatment to date, i.e. laser photocoagulation. However, the injections also provide an important added value, since, unlike lasers, they do not produce scars on the retina and thus maintain the visual field, sensitivity and contrast intact, resulting in better vision for the treated patients.
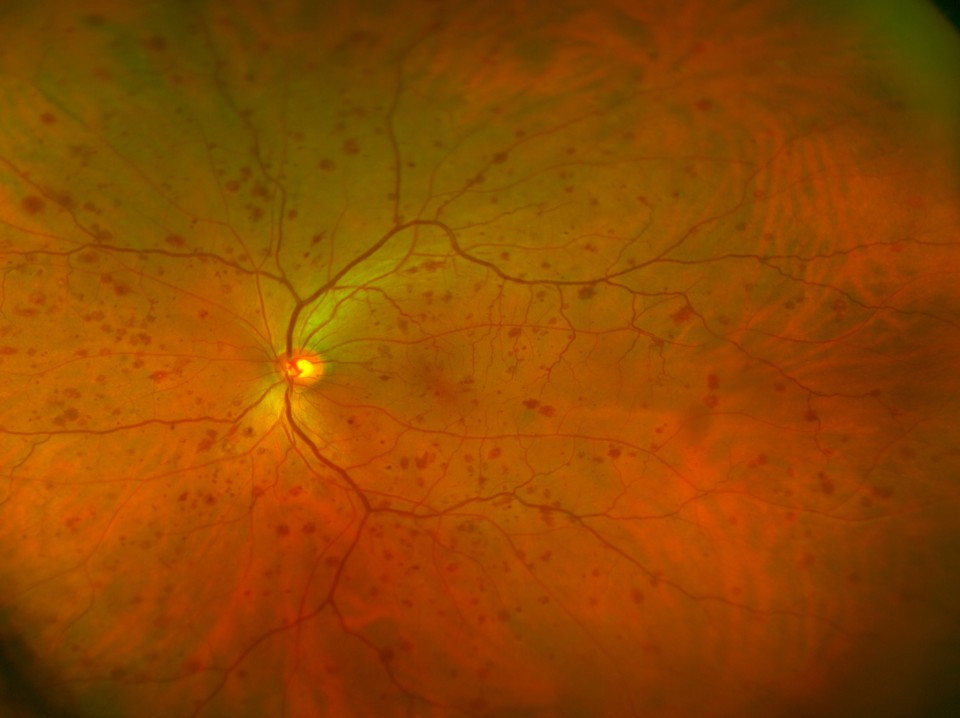
What is diabetic retinopathy
Diabetic retinopathy is the disease suffered by diabetic patients in the fundus of the eye, affecting the most sensitive eye tissue, which is the retina, a highly vascularised structure with very thin vessels, which makes it highly vulnerable to changes in pressure, blood glucose and other cardiovascular factors. Specifically, diabetic retinopathy can appear as vision loss and, if not controlled, can lead to blindness in very advanced cases.
Symptoms of diabetic retinopathy
In mild stages of the disease, the patient may not show any symptoms and, for this very reason, may abandon control of their eye disease, a neglect that is worsened by the fact that “the diabetic patient has many other pathologies apart from that of the eye, so they should attend appointments with their endocrinologist, perhaps with their cardiologist, etc. As they see well, they often stop seeing the ophthalmologist, who can detect anomalies that do not cause symptoms and can be treated,” warns the Miranza IOA specialist.
As diabetic retinopathy progresses, the retinal vessels start to show incompetence, causing haemorrhage or fluid leakage that accumulates in the retina and causes vision loss. “Both patients and ophthalmologists need to be very vigilant about these symptoms in order to detect the disease as soon as possible.”
The most common complication and leading cause of blindness among these patients is diabetic macular oedema, which affects around 25% of patients with diabetic retinopathy and is located in the central part of the retina, causing loss of vision, blurred or distorted vision. Dr Asencio explains that “although we cannot cure the disease, we can keep it at bay so that the patient does not continue to lose vision.”