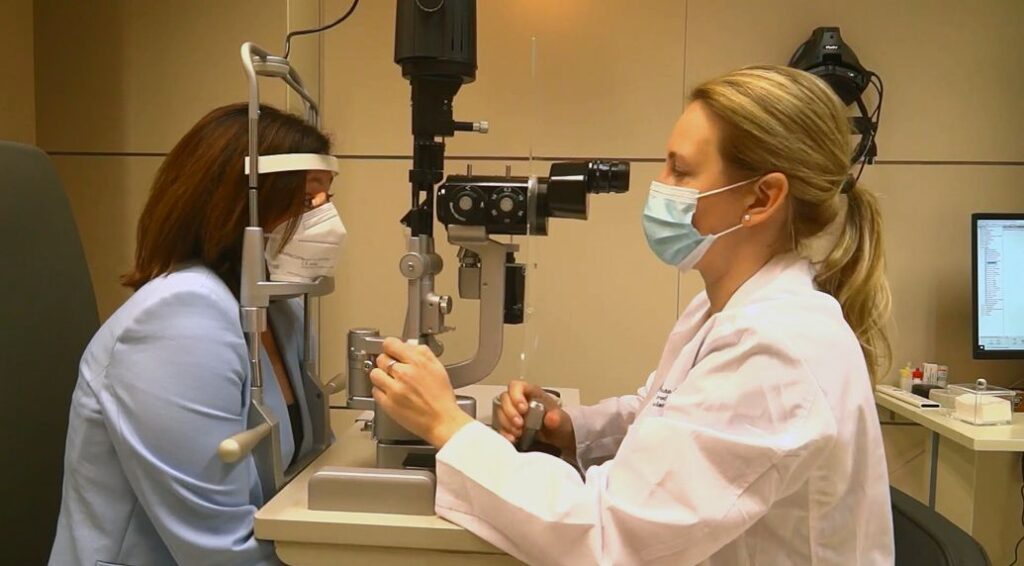
The swelling due to diabetes conditions ophthalmological treatments and vision recovery
Moreover, 5% of patients with diabetes still go to the ophthalmologist when their disease is already advanced and their sight requires urgent surgery.
Although the treatment of vision complications secondary to diabetes has evolved greatly in the last three decades, this disease, which affects more than 6 million people in Spain, still is a challenge for ophthalmologists. “There is increasing evidence that diabetes not only features a vascular component, but also a neurotrophic and inflammatory one. This causes the visual recovery of patients after undergoing treatment to be slower, unstable and unpredictable, while varying greatly from one person to another, regardless of the degree of severity of the disease”, explains Dra. Andrea Oleñik, a specialist at IMO Grupo Miranza.
This is reflected, for instance, in vitrectomy, the most common surgery to treat problems of the eye fundus, whose final results in vision, in the case of diabetics, can last from 1-2 weeks, as is usually the case, up to several months. Furthermore, “the risk of visual relapses also increases when there are inflammatory episodes or chronic underlying inflammation associated with diabetes”, says Dr Oleñik, who stresses the importance of paying attention to this aspect and managing it properly in the ophthalmological office with either topical (drops) or intravitreal anti-inflammatory drugs.
On the other hand, a customised study and follow-up of the eyesight of each patient with diabetes is also essential and, according to Dr Oleñik, “as ophthalmologists, we should not focus only on the eye, but on the patient as a whole, taking into account their general state of health.”
A comprehensive approach to the effect of diabetes on vision
Studies have shown that the presence of diabetic retinopathy (retinal damage caused by diabetes) and diabetic nephropathy (kidney damage) are mutually related, which highlights the importance of cooperation with different healthcare professionals, such as endocrinologists and nephrologists. Dr Oleñik warns that “within ophthalmology, we must also bear in mind that the retina is not the only area affected by diabetes, which can also affect the optic nerve by depleting its nerve fibres and the cornea by producing ulcers. All of these structures are essential for vision.”
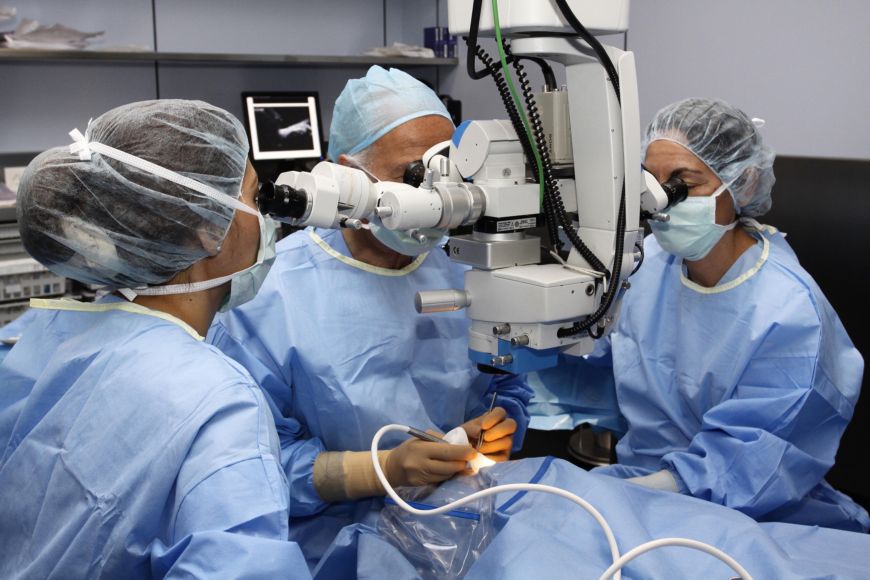
The preventive culture of diabetic patients
Our specialists stress that 5% of visits to the ophthalmologist due to diabetes affecting vision occur when the eye damage is already advanced and can leave irreversible visual consequences. They are mainly young, insulin-dependent patients with type 1 diabetes who, due to lack of awareness or other constraints, have poor metabolic control. In fact, patients with complex diabetes who, despite taking appropriate preventive measures, severely lose vision represent less than 1% (as is the case of Cris de Diego), which highlights the importance of prevention.
Along with therapeutic innovation in terms of drugs, laser and surgery, follow-up programmes and early detection of visual problems in patients with diabetes are key to avoid the development of eye complications. Thus, Miranza recommends a check-up with the ophthalmologist at least once a year, if you have diabetes, or more frequently, at the intervals indicated by the specialist, if some degree of diabetic retinopathy has already been diagnosed. Globally, this still remains the leading cause of blindness in working-age adults.